By Kim Smiley
Recently, increasing amounts of information has been released regarding patients suffering from tissue death (purpura) associated with use of cocaine “cut” (contaminated) with levamisole. Levamisole is a veterinary anti-worming drug no longer used in humans because of adverse side effects (such as the tissue death described above and also its interference with the blood marrow’s ability to produce white blood cells, known as agranulocytosis). The US Drug Enforcement Agency (DEA) reported in 2009 that 69% of cocaine was contaminated, a significant increase from previous years.
This issue can be examined within a root cause analysis captured in visual form. To begin, we capture the impacts to the goals. The patient safety goal is impacted because of the tissue death. Additionally, employees and patient services are impacted because many healthcare organizations are unable to diagnose the issue. We begin with these goals and ask “Why” questions to continue the analysis.
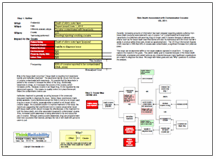 Why is the tissue death occurring? Tissue death is resulting from levamisole toxicity and ineffective treatment. The levamisole toxicity occurs from the use of cocaine contaminated with levamisole. It’s possible that the levamisole is added to the cocaine to increase the effect of the drug. Additionally, levamisole is cheap, so it increases the volume of the cocaine, which increases profits. Because cocaine is an illegal drug, it’s not regulated by any government agency. This means no quality control is in place that would detect the contamination before use.
Why is the tissue death occurring? Tissue death is resulting from levamisole toxicity and ineffective treatment. The levamisole toxicity occurs from the use of cocaine contaminated with levamisole. It’s possible that the levamisole is added to the cocaine to increase the effect of the drug. Additionally, levamisole is cheap, so it increases the volume of the cocaine, which increases profits. Because cocaine is an illegal drug, it’s not regulated by any government agency. This means no quality control is in place that would detect the contamination before use.
Ineffective treatment is generally occurring because of the previously discussed inability to diagnose the issue. Before these reports were made widely available, most practitioners would not think to look at a no-longer-used drug as a cause of toxicity, especially when a patient is not honest about cocaine usage. As a possible solution to improve treatment of this issue, the reports are suggesting that practitioners look to cocaine abuse when faced with tissue death, which should increase the effectiveness of the treatment for both the tissue death, and other associated issues with contaminated cocaine. Also, increased public awareness is being attempted to try and reduce the use of cocaine. Although previous public awareness drug use programs have been less successful than desired, perhaps the risk of skin death will get some users to quit.
For more information, click here.


 Some of the more common issues that lead to medication errors include confusion on the label of the medication. It is estimated that almost half of Americans don’t understand the dosing instructions on their medication, leading to the potential for medication dosing errors. It’s no wonder, when “take one pill a day,” can be written in 44 different ways according to Dr. Ruth Parker. Additionally, many patients receive medication instructions that are either not in their primary language, or contain errors in the translation (see our previous blog about errors
Some of the more common issues that lead to medication errors include confusion on the label of the medication. It is estimated that almost half of Americans don’t understand the dosing instructions on their medication, leading to the potential for medication dosing errors. It’s no wonder, when “take one pill a day,” can be written in 44 different ways according to Dr. Ruth Parker. Additionally, many patients receive medication instructions that are either not in their primary language, or contain errors in the translation (see our previous blog about errors 
