One of the most exciting moments in a young couples’ relationship is finding out that they are about to start a family. New moms-to-be will take extra precautions to make sure their child has the best possible start in life – a healthier diet, a regimen on prenatal vitamins, limitations on coffee and so on. However, that excitement is sometimes tempered with worry about the new baby’s health.
Mareena Silva had just found out she was expecting. Six weeks pregnant and a bit under the weather, her doctor prescribed Mareena antibiotics to clear up an infection. She filled the prescription at the local Safeway, and after taking the medicine as directed, became nauseous. Upon checking the medication label, she made the horrifying discovery that she had been given the wrong medicine.
 Instead of the antibiotics she had been prescribed, Mareena had taken a dose of methotrexate. Methotrexate is a chemotherapy drug which targets rapidly dividing cells, like cancer…or embryos. Her doctor urged her to vomit whatever medicine she could. Then an ambulance rushed her to the hospital where she was given charcoal to absorb any medication remaining in her stomach. Unfortunately, at this point all she can do is wait to see if her unborn child was affected by the unintended medication. Methotrexate can cause serious birth defects, especially during the critical formative period during the first trimester, and even miscarriage. Reports state that the baby faces 50-50 odds of developing abnormalities.
Instead of the antibiotics she had been prescribed, Mareena had taken a dose of methotrexate. Methotrexate is a chemotherapy drug which targets rapidly dividing cells, like cancer…or embryos. Her doctor urged her to vomit whatever medicine she could. Then an ambulance rushed her to the hospital where she was given charcoal to absorb any medication remaining in her stomach. Unfortunately, at this point all she can do is wait to see if her unborn child was affected by the unintended medication. Methotrexate can cause serious birth defects, especially during the critical formative period during the first trimester, and even miscarriage. Reports state that the baby faces 50-50 odds of developing abnormalities.
How did Mareena end up with a drug sometimes used to abort ectopic pregnancies? The pharmacy staff dispensing the medication accidentally handed her one intended for patient in her late 50’s with a very similar name. According to statements released by Safeway, pharmacy staff failed to repeat Silva’s name to her twice and verify her birth date – standard company policy. The company has said that they are conducting an investigation to see why their procedure was not followed. They will not be the only ones looking into the incident; the Colorado Pharmacy Board will also be reviewing the case.
Unfortunately mistakes like this are far too common. No national agency tracks how many prescriptions are incorrectly distributed, and few states track such information either. However, a 2003 study by Auburn University indicates that the dispensing error rate could conservatively be estimated at 1%. That’s astonishing considering billions of prescriptions are filled each year. How might those errors be prevented? Dispensing medication is more complex than meets the eye, and there are a number of places a mistake can happen. In this instance, Safeway’s pharmaceutical staff did not follow proper procedures for dispensing medication. 18.3% of dispensing errors were caused by procedures not followed according to U.S. Pharmacopeia’s 2003 study of medication error reports.
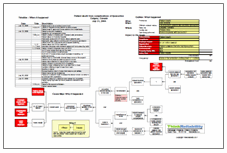
While the investigation will unearth further information about what happened behind the counter that day, a detailed Cause Map pictorially lays out how the incident occurred and why. As the investigation unfolds, more information can be added and solutions can be developed to prevent future incidents like this one from happening.