In previous blogs, we wrote about nonketotic hyperosmolar coma and diabetic ketoacidosis, which are both conditions related to hyperglycemia, or high blood glucose. In this blog, we consider the last type of manifestation of poor glycemic control that, when it occurs in the hospital, is considered a hospital-acquired condition by Medicare & Medicaid, meaning that hospitals will not receive additional payment for cases when this condition is acquired during hospitalization. Hypogelycemic coma, along with nonketotic hyperosmolar coma and diabetic ketoacidosis, results from poor glycemic control within the hospital, but is caused by low blood glucose.
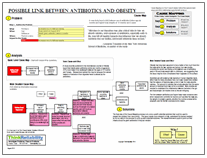
As we did with the other two manifestations of poor glycemic control, we can look at the impacted goals for a hospital and the potential causes and solutions for this condition in a visual root cause analysis or Cause Map. The goals for hypoglycemic coma are the same to the other manifestations of poor glycemic control and include increased risk of patient death, length of patient stay and treatment needs. The costs associated with hypoglycemic coma (greater than $7 million in the US from the 212 cases reported to CMS in 2007) are no longer reimbursable when the condition is acquired in the hospital. There is also always the potential that a patient death can result in a second victim – the patient’s provider(s).
 Hypoglycemic coma results from uncontrolled hypoglycemia, which can result from overtreatment with insulin, drug-induced hypoglycemia, drug interaction with insulin, decreased glucose production and/or loss of glucose. Overtreatment with insulin was implicated in 90% of hypoglycemia cases in a recent study and can result from medication errors (see our analysis on medication errors in hospital settings), or a failure to adjust insulin for diet or other factors. Drug-induced hypoglycemia can result from administration of fluoroquinolones (the mechanism for this effect is unknown) and/or inadequate nutrition. Drugs that interact with insulin may be administered to a diabetic patient if providers are lacking in knowledge about glycemic control. Underlying disease or infection, such as chronic renal insufficiency, which was implicated in approximately 50% of hypoglycemia cases in the study, can result in decreased glucose production or loss of glucose.
Hypoglycemic coma results from uncontrolled hypoglycemia, which can result from overtreatment with insulin, drug-induced hypoglycemia, drug interaction with insulin, decreased glucose production and/or loss of glucose. Overtreatment with insulin was implicated in 90% of hypoglycemia cases in a recent study and can result from medication errors (see our analysis on medication errors in hospital settings), or a failure to adjust insulin for diet or other factors. Drug-induced hypoglycemia can result from administration of fluoroquinolones (the mechanism for this effect is unknown) and/or inadequate nutrition. Drugs that interact with insulin may be administered to a diabetic patient if providers are lacking in knowledge about glycemic control. Underlying disease or infection, such as chronic renal insufficiency, which was implicated in approximately 50% of hypoglycemia cases in the study, can result in decreased glucose production or loss of glucose.
As with the other types of manifestations of poor glycemic control, efforts must be made to prevent these types of incidents. As suggested with hyperglycemic events, insulin plans should be individualized, accounting for all relevant factors related to glycemic control and diet. Patients treated with insulin in the hospital should have their blood glucose levels monitored frequently, especially as insulin has been identified as a High-alert medication by The Joint Commission. Any patients found unconscious should also immediately have their blood glucose levels measured. Patient’s nutritional intake must be carefully monitored, especially for cases involving medications that might cause hypoglycemia. Last but not least, controls and procedures involving drugs given to diabetic patients should be carefully controlled, due to the high potential and risk for interaction with insulin.
Two other conditions are considered hospital-acquired manifestations of poor glycemic control: nonketotic hyperosmolar coma and diabetic ketoacidosis. In previous blogs, we discussed the causes of these issues, and suggested solutions to reduce the risk of these types of incidents.
To view the Outline, Cause Map, and Potential Solutions, please click “Download PDF” above. Or click here to read more.


 According to a
According to a