A gas tanker was providing fuel to a maternity hospital in Mexico City when the gas workers discovered a leak. They contacted the fire department, had the hospital evacuated, and attempted to put out the leak. Unfortunately, the leaked gas exploded, killing at least 2 nurses and 2 babies, and leveling most of the hospital.
Dozens more infants, patients and nursing staff were injured, along with the three gas workers present at the scene. The gas workers have all been arrested, though the charges against them have not been released. While it appears that the workers are being held responsible for the tragedy, providing an objective, factual analysis as to what happened can provide useful information to reduce the risk of the issue happening again.
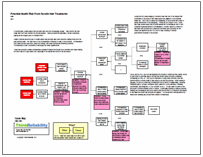
When performing a root cause analysis of an issue (as we will do here in a Cause Map), it’s important to first capture the impacts to the organizational goals as a result of the incident being investigated. In this case, the patient safety goal is impacted because of the deaths of two infants and the injuries to dozens of patients. The safety of hospital employees was impacted due to the deaths of two nurses and injuries to many more. Additionally, the safety of the gas company employees was impacted because all three of the gas workers were injured.
The environment was impacted due to the gas leak. The compliance goal was impacted because the three workers were arrested. The patient services and operations goals were impacted by the evacuation from the hospital (which is very difficult on patients and staff, although it likely saved many lives in this case). The property goal is impacted because of the severe damage to the hospital and the labor goal is impacted by the rescue efforts. (Hospital neighbors are reported to have provided considerable assistance to the rescue efforts at no small risk to themselves.)
Any time deaths or injuries result from an explosion, it is important not only to determine what caused the explosion, but whether the response could have been improved. In this case, the explosion occurred while the hospital was being evacuated, though a specific timeline of the leak, evacuation and explosion has not been released. Further analysis into the evacuation will help determine whether improvements could have saved lives.
In the case of the explosion, the fuel was provided by the leaked gas. Adequate oxygen was present in the air, and the ignition source (heat) could have been provided by hospital operations (the gas was being delivered near the hospital kitchen) or potentially by work being done to repair the leak (such as static or a spark). The gas leaked due to a faulty gas delivery hose. When a faulty part contributes to a tragedy such as this one, it’s important to determine not only how the damage occurred (if possible), but whether inspections or maintenance could have reduced the risk of an incident. Clearly if the hose had been discovered to be faulty and replaced before the delivery took place, the risk of an explosion would have been greatly decreased.
A broader issue for the entire country is the question of why gas leaks and explosions are fairly common. Part of this is because there is no infrastructure to pipe gas underground and it instead has to be delivered by truck. A similar incident involving a hose issue on a gas truck killed three in Queretaro in July last year. The company that provided the gas to the hospital in this case says that it has 1,000 trucks that deliver gas to over 80% of the country. With such a large distribution network, accidents are bound to happen. However, clearly more effort needs to go into making sure that the impact on human lives is reduced.